Biopharma/Biotech Annual Report 2021 – Life after COVID-19: “New Normal”
Life after COVID-19: “New Normal”
With more than half of the U.S. population fully vaccinated and mask mandates being lifted throughout the country, America looks to resume “normal life” before the pandemic took over.
By Andrew Humphreys • [email protected]
The United States had administered about 297 million doses of COVID-19 vaccines and distributed 367 million doses in the country as of June 2, based on data from the Centers for Disease Control and Prevention. According to the agency as of that date, 168,734,435 people had received at least one dose while 136,155,250 people were fully vaccinated. The CDC tally includes two-dose vaccines from Moderna Inc. and Pfizer Inc./BioNTech SE, as well as Johnson & Johnson’s one-shot vaccine. The White House is accelerating efforts to get 70 percent of U.S. adults vaccinated against COVID-19 with at least one shot by July 4.
Pfizer/BioNTech and AstraZeneca Plc are set to lead global COVID-19 vaccine supplies for 2021, estimates from Airfinity Ltd. indicated as of the end of May. By the end of 2021, the production of COVID-19 vaccines could reach ~11.1 billion doses across the world, the London-based research company projected, with assumptions including the potential regulatory authorizations for shots undergoing late-stage studies.
Noting ~10.8 billion doses are necessary to vaccinate 75 percent of the world’s population aged 5 years and older, the estimates suggest that “enough vaccine will have been produced this year to reach herd immunity worldwide,” according to the researchers. BNT162b2 from Pfizer/BioNTech (~2.5 billion doses) and AZD1222 from AstraZeneca (~2.0 billion doses) are expected to lead 2021 COVID-19 vaccine supplies followed by ~1.4 billion doses of CoronaVac from Sinovac Biotech.
However, the researchers additionally highlight the inequitable access to vaccines noting that six countries led by the EU and the United Sates hold an estimated ~89.7 percent of the likely surplus of vaccines which is projected at more than 2.6 billion doses, analysts from Seeking Alpha point out. “The estimates do not include any upside to production that could result from a potential waiver on COVID-19 vaccine patents. The move supported by the United States met with strong opposition from global pharmaceutical companies this month (May),” according to Seeking Alpha.
Outside of the “Big Three” COVID-19 vaccines from Pfizer/BioNTech, Moderna, and J&J being administered in the United States along with other companies’ shots being used internationally, another one to watch on the global front is Novavax Inc.’s NVX-CoV2373. Engineered from the genetic sequence of COVID-19, Novavax used the company’s recombinant nanoparticle technology to generate antigen derived from the coronavirus spike protein. In combination with the company’s proprietary Matrix-M adjuvant, NVX-CoV2373 has shown in studies that it binds efficiently with human receptors targeted by the virus, a critical aspect for effective vaccine protection.
NVX-CoV2373 is being assessed in two pivotal Phase III trials: a study in the United Kingdom that completed enrollment in November and the PREVENT-19 trial in the United States and Mexico that started during December. NVX-CoV2373 is additionally being evaluated in two Phase II trials that began in August: a Phase IIb study in South Africa, and a Phase I/II continuation in the United States and Australia.
Earlier this year, Novavax announced a final analysis of data from the company’s Phase III study in the U.K. for the protein-based COVID-19 vaccine candidate, demonstrating an overall efficacy of 90 percent and confirming the vaccine’s efficacy against variants. The data from the U.K. late-stage trial and South Africa Phase IIb study were the first to show clinical efficacy against newer circulating U.K. and South Africa COVID-19 variants.
According to Novavax, NVX-CoV2373 contains purified protein antigen and can neither replicate, nor can it cause COVID-19. In preclinical studies, NVX-CoV2373 induced antibodies that blocked the binding of spike protein to cellular receptors and provided infection and disease protection. The vaccine candidate was generally well-tolerated and elicited robust antibody response in Phase I/II tests.
The U.K. study demonstrated efficacy of 96.4 percent against the original virus strain, 86.3 percent against the B.1.1.7/501Y.V1 variant, and 89.7 percent overall. The Phase IIb study in South Africa demonstrated 48.6 percent efficacy against a newly emerging escape variant first described in that country.
In May, Novavax again delayed the company’s timeline for ramping up COVID-19 vaccine production due to manufacturing obstacles and said it does not expect to seek regulatory authorization for the shot in the United States, Britain and Europe until third-quarter 2021. Novavax does not expect to hit the company’s production target of 150 million shots per month until fourth-quarter 2021, later than the previous Q3 forecast. The Gaithersburg, Md.-based company previously said it could receive U.S. regulatory authorization as soon as May 2021.
NOVEL DRUG APPROVALS DURING 2021
As companies around the world continue to devote significant R&D expenses to develop and improve vaccines and antibody therapeutics to combat the novel coronavirus, the U.S. Food and Drug Administration’s Center for Drug Evaluation and Research (CDER) during the first five months of 2021 approved 24 new molecular entities and new therapeutic biological products, including innovative products that never have been used in clinical practice. During January-May 2021, the FDA’s Center for Biologics Evaluation and Research (CBER) approved two Biologics License Applications (BLAs). The following section highlights some of the New Drug Applications (NDAs) and BLAs granted marketing clearance by CDER during the first five months of 2021.
First approved targeted therapy for tumors with any KRAS mutation
 The U.S. FDA on May 28 approved Lumakras (sotorasib) as the first treatment for adult patients with non-small cell lung cancer whose tumors have a specific type of genetic mutation called KRAS G12C and who have received at least one prior systemic therapy. Lumakras represents the first approved targeted therapy for tumors with any KRAS mutation, which accounts for 25 percent of mutations in non-small cell lung cancers. KRAS G12C mutations represent about 13 percent of mutations in non-small cell lung cancers (NSCLC).
The U.S. FDA on May 28 approved Lumakras (sotorasib) as the first treatment for adult patients with non-small cell lung cancer whose tumors have a specific type of genetic mutation called KRAS G12C and who have received at least one prior systemic therapy. Lumakras represents the first approved targeted therapy for tumors with any KRAS mutation, which accounts for 25 percent of mutations in non-small cell lung cancers. KRAS G12C mutations represent about 13 percent of mutations in non-small cell lung cancers (NSCLC).
“KRAS mutations have long been considered resistant to drug therapy, representing a true unmet need for patients with certain types of cancer,” said Richard Pazdur, M.D., director of the FDA’s Oncology Center of Excellence and acting director of the Office of Oncologic Diseases in the FDA’s Center for Drug Evaluation and Research. “The approval represents a significant step towards a future where more patients will have a personalized treatment approach.”
Lumakras was approved using the Accelerated Approval pathway, under which the regulatory agency may approve medicines for serious conditions where there is unmet medical need and a drug is shown to have certain effects that are reasonably likely to predict a clinical benefit to patients. Additional study is required to verify and describe anticipated clinical benefits of Lumakras, which is administered as a 960-milligram pill once per day.
The FDA granted the Lumakras application Fast Track, Priority Review, and Breakthrough Therapy designations. The product additionally received Orphan Drug designation, which provides incentives to assist and encourage the development of drugs for rare diseases.
The U.S. regulatory review was conducted under Project Orbis, an initiative of the FDA Oncology Center of Excellence. Project Orbis provides a framework for concurrent submission and review of oncology medicines among international partners.
FDA approval of Lumakras was granted to Amgen Inc. U.S. regulators also approved the Qiagen therascreen KRAS RGQ PCR kit and the Guardant360 CDx as companion diagnostics for Lumakras. The Qiagen GmbH test analyzes tumor tissue and the Guardant Health Inc. test analyzes plasma specimens to determine if Lumakras is an appropriate treatment for patients. If no mutation is detected in a plasma specimen, the patient’s tumor should be tested.
“The FDA approval of Lumakras is a breakthrough moment for patients with KRAS G12C-mutated non-small cell lung cancer because there is now a targeted therapy for this common, but previously elusive, mutation,” said David M. Reese, M.D., executive VP of R&D at Amgen. “KRAS has challenged cancer researchers for more than 40 years with many deeming it as ‘undruggable.’ The Lumakras development program was a race against cancer for Amgen’s scientists and clinical trial investigators who together have now successfully delivered this new medicine to patients in less than three years – from first patient dosed to U.S. regulatory approval.”
According to reports, the Amgen drug will have a monthly U.S. list price of $17,900 and Wall Street analysts, on average, project 2022 sales of $240 million. By 2026, annual sales have been projected to reach $1.51 billion.
First targeted treatment for NSCLC subset
One week before the Lumakras approval, Janssen’s  was granted U.S. marketing clearance as the first targeted treatment for patients with non-small cell lung cancer (NSCLC) with EGFR exon 20 insertion mutations. Rybrevant represents the first fully human, bispecific antibody approved in lung cancer. The U.S. regulatory agency simultaneously approved Guardant Health’s Guardant360 CDx liquid biopsy blood test as a companion diagnostic for use with Rybrevant.
was granted U.S. marketing clearance as the first targeted treatment for patients with non-small cell lung cancer (NSCLC) with EGFR exon 20 insertion mutations. Rybrevant represents the first fully human, bispecific antibody approved in lung cancer. The U.S. regulatory agency simultaneously approved Guardant Health’s Guardant360 CDx liquid biopsy blood test as a companion diagnostic for use with Rybrevant.
The FDA granted accelerated approval of Rybrevant (amivantamab-vmjw) for treating adult patients with locally advanced or metastatic non-small cell lung cancer with epidermal growth factor receptor (EGFR) exon 20 insertion mutations, as detected by an FDA-approved test, whose disease has progressed on or after platinum-based chemotherapy. Rybrevant is the first fully human, bispecific antibody approved for treating patients with NSCLC that targets EGFR exon 20 insertion mutations, which are the third most prevalent activating EGFR mutation. The U.S. approval follows the FDA’s decision to grant Breakthrough Therapy Designation (BTD) during March 2020 and to initiate a Priority Review of the Biologics License Application in December 2020.
Lung cancer is the top cause of cancer death among men and women, accounting for nearly 25 percent of all cancer deaths. Previously approved targeted treatments, including EGFR tyrosine kinase inhibitors (TKI) are generally insensitive in treating NSCLC driven by EGFR exon 20 insertion mutations and are not FDA-approved for these patients. Additionally, NSCLC driven by this mutation carries a worse prognosis and shorter survival rates versus lung cancer driven by more common EGFR mutations, such as exon 19 deletions and L858R substitutions. Patients newly diagnosed with metastatic NSCLC with EGFR exon 20 insertion mutations have a real-world median overall survival of 16.2 months, which is lower than patients with EGFR exon 19 deletions/L858R mutations, who have a real-world median OS of 25.5 months.
The fully human bispecific antibody directed against EGFR and MET receptors binds extracellularly (outside of the cell), inhibiting tumor growth and leading to tumor cell death. While other TKIs including AstraZeneca’s market-leader Tagrisso hit EGFR from within the cell, Rybrevant attacks from the outside, allowing it to bypass resistance to existing TKIs.
“Advances in precision oncology continue to facilitate drug development, allowing diseases like lung cancer to be subset into biomarker-defined populations appropriate for targeted therapies,” said Julia Beaver, M.D., chief of medical oncology in FDA’s Oncology Center of Excellence and acting deputy director of the Office of Oncologic Diseases in CDER. “With the approval, for the first time, patients with non-small cell lung cancer with EGFR exon 20 insertion mutations will have a targeted treatment option.”
First FDA-approved targeted C3 therapy
The FDA on May 14 approved  (pegcetacoplan) injection for the treatment of adults with paroxysmal nocturnal hemoglobinuria (PNH), a rare, life-threatening blood disease. Empaveli is the first PNH treatment that binds to complement protein C3. The drug is approved for use in adults with PNH who are treatment-naïve as well as patients switching from the C5 inhibitors Soliris (eculizumab) and Ultomiris (ravulizumab).
(pegcetacoplan) injection for the treatment of adults with paroxysmal nocturnal hemoglobinuria (PNH), a rare, life-threatening blood disease. Empaveli is the first PNH treatment that binds to complement protein C3. The drug is approved for use in adults with PNH who are treatment-naïve as well as patients switching from the C5 inhibitors Soliris (eculizumab) and Ultomiris (ravulizumab).
The FDA granted marketing approval of the new medicine to Apellis Pharmaceuticals. Empaveli was granted Priority Review, Fast Track, and Orphan Drug designations for the approved indication.
“As the first, FDA-approved targeted C3 therapy, Empaveli has the potential to redefine treatment for adults with PNH, including patients switching from any C5 inhibitor and treatment-naïve patients,” said Cedric Francois, M.D., Ph.D., co-founder and CEO of Apellis. “This approval represents a major scientific advancement as Empaveli ushers in the first new class of complement medicine in almost 15 years. We look forward to exploring the full potential of targeting C3 and continue to advance registrational programs of this therapy across multiple complement-driven diseases with high unmet need.”
Paroxysmal nocturnal hemoglobinuria is characterized by red blood cell destruction, anemia (red blood cells unable to carry enough oxygen to tissues), blood clots, and impaired bone marrow function (not making enough blood cells). PNH is caused by gene mutations that affect red blood cells. Red blood cells in people with these mutations are defective and can be destroyed by the immune system, which results in anemia.
The U.S. approval of Empaveli is based on results from the head-to-head Phase III PEGASUS trial, which were published in the New England Journal of Medicine. In the PEGASUS trial, Empaveli met the primary endpoint, showing superiority to Soliris for the change from baseline in hemoglobin level at Week 16 with an adjusted mean increase of 3.84 g/dL of hemoglobin (p<0.0001). Empaveli met non-inferiority compared to Soliris on the endpoint of transfusion avoidance. Eighty-five percent of Empaveli-treated patients were transfusion free over 16 weeks versus 15 percent of Soliris-treated patients. Alexion Pharmaceuticals’ Soliris (eculizumab) has been evaluated in 51 clinical studies and is FDA-approved for the treatment of four different complement-related diseases.
First CD19-targeted ADC as single-agent treatment for r/r DLBCL
 Zynlonta won U.S. marketing clearance on April 23 as the first CD19-targeted antibody drug conjugate (ADC) as a single-agent treatment for adult patients with relapsed or refractory (r/r) diffuse large B-cell lymphoma (DLBCL). Zynlonta was granted accelerated approval by U.S. regulators based on overall response rate.
Zynlonta won U.S. marketing clearance on April 23 as the first CD19-targeted antibody drug conjugate (ADC) as a single-agent treatment for adult patients with relapsed or refractory (r/r) diffuse large B-cell lymphoma (DLBCL). Zynlonta was granted accelerated approval by U.S. regulators based on overall response rate.
DLBCL is the most common type of non-Hodgkin lymphoma in the United States. DLBCL is a rapidly progressing, aggressive disease that is heterogeneous with multiple subtypes. More than 40 percent of first-line DLBCL treatments fail, according to data.
“There is a significant unmet need for treatment options for patients with r/r DLBCL, including those who have been heavily pretreated and have difficult-to-treat disease,” stated Paolo F. Caimi, M.D., University Hospitals Cleveland Medical Center and Case Comprehensive Cancer Center, Case Western Reserve University. “Single-agent Zynlonta demonstrated clinically important outcomes in the pivotal LOTIS-2 study across several disease subtypes. Notably, this included transplant eligible and ineligible patients and patients who previously received stem cell transplant or CAR-T cell therapy.”
ADC Therapeutics launched the Advancing Patient Support Program, a comprehensive patient support program offering financial assistance, ongoing education and other resources to eligible patients.
First novel non-stimulant ADHD treatment in a decade
Supernus Pharmaceuticals Inc. was the recipient of FDA approval on April 2 for Qelbree for treating attention-deficit hyperactivity disorder in pediatric patients 6 to 17 years of age. Qelbree (viloxazine extended-release capsules) represents the first novel non-stimulant treatment for ADHD in a decade and was made available in the United States in second-quarter 2021.
“Based on the efficacy demonstrated in the clinical program, we believe Qelbree offers a unique new alternative for the treatment of ADHD,” said Jack A. Khattar, president and CEO of Supernus. “Qelbree provides prescribing physicians and patients living with ADHD a therapy that is not a controlled substance with proven efficacy and a tolerable safety profile. We are grateful to the patients, families and their care givers who participated in and supported our research.”
The U.S. marketing clearance is supported by clinical data from an extensive development program consisting of four Phase III studies that evaluated more than 1,000 pediatric patients from the age of 6 to 17 years. In December 2020, Supernus announced positive results from a Phase III trial in adults with ADHD and plans to file a supplemental New Drug Application to the FDA for Qelbree in adults during second-half 2021.
“ADHD is one of the most common mental health issues in the U.S.,” noted Andrew J. Cutler, M.D., Clinical Associate Professor of Psychiatry at SUNY Upstate Medical University, and Chief Medical Officer, Neuroscience Education Institute. “The right treatment is key for children and adolescents, as they grow and navigate school and social relationships. This approval offers a novel once-a-day sprinkleable non-stimulant that can be a great option for children and adolescents with ADHD.”
Qelbree’s U.S. marketplace competition includes various generic drugs, Eli Lilly and Co.’s Strattera, and Shire Plc’s Intuniv, which was the last branded, non-scheduled ADHD to win FDA approval during 2009. According to industry analysts, Qelbree evidently avoids the rare liver toxicity concerns of Strattera and the hypotension concerns of Intuniv.
First FDA-approved oral disease modifying therapy studied against established oral comparator
Johnson & Johnson/Janssen’s newly approved drug Ponvory (ponesimod) for adults with relapsing multiple sclerosis launched in the United States during early April 2021. The once-daily oral selective sphingosine-1-phosphate receptor 1 (S1P1) modulator was cleared for U.S. marketing on March 18 to treat adults with relapsing forms of MS to include clinically isolated syndrome, relapsing-remitting disease and active secondary progressive disease. The medicine offers MS patients superior efficacy in reducing annualized relapse rates versus an established oral therapy and a proven safety profile backed by more than a decade of cumulative clinical research.
Ponvory is the first FDA-approved oral disease modifying therapy studied against an established oral comparator. The approval follows more than 10 years of cumulative data showing the treatment’s efficacy and safety. Head-to-head pivotal study results demonstrated Ponvory treatment resulted in nearly a third fewer annual relapses than teriflunomide, marketed as Aubagio by Sanofi Genzyme.
Ponvory is believed to work by keeping immune cells known as lymphocytes out of the blood by trapping them in the lymph nodes. The way the medicine exerts therapeutic effects in multiple sclerosis is unknown, but may help keep the lymphocytes out of the central nervous system, where they could cause damage.
A member of the Janssen Pharmaceutical Companies of J&J, Actelion Pharmaceuticals Ltd. is party to a revenue sharing agreement with Idorsia Pharmaceuticals Ltd., which provides for certain payments to Idorsia related to ponesimod sales.
At the time of launch, Ponvory was the newest S1P1 modulator entrant for MS in the U.S. marketplace, joining Novartis AG’s Gilenya and that drug’s follow-on Mayzent along with Bristol Myers Squibb Co.’s Zeposia. Near the end of May 2021, Zeposia gained a second indication from the FDA, becoming the first S1P1 receptor modulator approved for ulcerative colitis. The once-daily oral medication was approved for patients with moderately to severely active UC.
First approved therapy to reduce risk of mortality in patients with MoCD Type A
 Nulibry (fosdenopterin) for injection was granted U.S. approval on Feb. 26 to reduce the risk of death due to molybdenum cofactor deficiency Type A. MoCD Type A is a rare, genetic, metabolic disorder that typically presents in the first few days of life, resulting in intractable seizures, brain injury and death. The median overall survival age is about four years.
Nulibry (fosdenopterin) for injection was granted U.S. approval on Feb. 26 to reduce the risk of death due to molybdenum cofactor deficiency Type A. MoCD Type A is a rare, genetic, metabolic disorder that typically presents in the first few days of life, resulting in intractable seizures, brain injury and death. The median overall survival age is about four years.
Nulibry is BridgeBio Pharma Inc.’s first FDA-approved therapeutic. The marketing application was awarded Priority Review and Breakthrough Therapy designations. Nulibry additionally received Orphan Drug designation, and BridgeBio affiliate Origin Biosciences Inc. was the recipient of a Rare Pediatric Disease Priority Review Voucher.
“The FDA’s approval of Nulibry means that patients with MoCD Type A and their families have an approved therapy for the first time. It also reflects our belief that every life matters and that no disease is too rare to address,” said BridgeBio founder and CEO Neil Kumar, Ph.D.
First myeloprotection therapy to help decrease incidence of chemotherapy-induced myelosuppression
 The FDA approved Cosela (trilaciclib) on Feb. 12 as the first therapy in the drug’s class to reduce the frequency of chemotherapy-induced bone marrow suppression in adults receiving certain types of chemotherapy for extensive-stage (when the cancer has spread beyond the lungs) small cell lung cancer. Cosela may help protect bone marrow cells from damage resulting from chemotherapy by inhibiting cyclin-dependent kinase 4/6, a type of enzyme.
The FDA approved Cosela (trilaciclib) on Feb. 12 as the first therapy in the drug’s class to reduce the frequency of chemotherapy-induced bone marrow suppression in adults receiving certain types of chemotherapy for extensive-stage (when the cancer has spread beyond the lungs) small cell lung cancer. Cosela may help protect bone marrow cells from damage resulting from chemotherapy by inhibiting cyclin-dependent kinase 4/6, a type of enzyme.
“For patients with extensive-stage small cell lung cancer, protecting bone marrow function may help make their chemotherapy safer and allow them to complete their course of treatment on time and according to plan,” stated Albert Deisseroth, M.D., Ph.D., supervisory medical officer in the Division of Non-Malignant Hematology in CDER. “The approval of Cosela will give patients a treatment option that can reduce the occurrence of a common, harmful side effect of chemotherapy.”
Cosela is the first therapy designed to help protect bone marrow when administered prior to treatment with chemotherapy. This is the only FDA-approved therapy that helps proactively deliver multilineage myeloprotection to patients with extensive-stage small cell lung cancer being treated with chemotherapy. Cosela is a 30-minute infusion administered within four hours of the beginning of chemotherapy.
G1 Therapeutics Inc. and Boehringer Ingelheim on March 2 announced that Cosela for injection was available in the United States. “This is an exciting time for the combined G1 and Boehringer Ingelheim team as we are now able to provide Cosela, the first proactive multilineage myeloprotection therapy, to patients with extensive-stage small cell lung cancer,” said Soma Gupta, Chief Commercial Officer at G1. “Our commitment includes ensuring excellence in support and access to Cosela; to that end, we are excited to launch the G1 to One Patient Support Program which is designed to provide access and affordability solutions to eligible patients.”
Trilaciclib is being studied across a range of tumor types and chemo regimens – small cell lung cancer , colorectal cancer, breast cancer and bladder cancer – to test the drug’s potential myeloprotection and antitumor efficacy and safety benefits combined with chemo.
First FDA-approved oral therapy for LN
Lupkynis is the first FDA-approved oral therapy for lupus nephritis (LN), a condition that causes irreversible kidney damage and increases the risk of kidney failure, cardiac events and death. The FDA cleared for marketing Aurinia Pharmaceuticals Inc.’s Lupkynis (voclosporin) in combination with a background immunosuppressive therapy regimen for the treatment of adults with active LN.
In pivotal studies, patients treated with Lupkynis in combination with standard-of-care (SoC) were more than twice as likely to achieve renal response and experienced a decrease in urine protein creatinine ratio twice as fast as patients on typical SoC alone. UPCR is a standard measurement used to monitor kidney protein levels. Patients treated with Lupkynis demonstrated improved response rates in all parameters across immunologically-active classes of LN studied.
According to Aurinia President and CEO Peter Greenleaf, “The approved label supports the efficacy and safety of Lupkynis as well as Aurinia’s proprietary and patented eGFR pharmacodynamic dosing protocol.”
First complete long-acting regimen for HIV treatment
Cabenuva is the first FDA-approved injectable, complete regimen for HIV-1 infected adults that is administered once monthly. The medicine contains ViiV Healthcare’s cabotegravir extended-release injectable suspension and Janssen’s rilpivirine extended-release injectable suspension, co-packaged for intramuscular use. Approved on Jan. 21, the FDA also gave the green light to Vocabria (cabotegravir) 30-mg tablets which should be taken in combination with oral rilpivirine (marketed as Edurant) for one month before starting treatment with Cabenuva to ensure the medications are well-tolerated before switching to the extended-release injectable formulation.
Lynn Baxter, Head of North America, ViiV Healthcare, stated, “The FDA approval of Cabenuva represents a shift in the way HIV is treated, offering people living with HIV a completely new approach to care. Cabenuva reduces the treatment dosing days from 365 days to 12 days per year. At ViiV Healthcare, we are dedicated to ensuring no one living with HIV is left behind, and adding this first-of-its-kind regimen to our industry-leading portfolio of innovative medicines reinforces our mission.”
The Cabenuva approval is based on the pivotal Phase III ATLAS (Antiretroviral Therapy as Long-Acting Suppression) and FLAIR (First Long-Acting Injectable Regimen) trials that included more than 1,100 patients from 16 countries. Cabenuva was preferred by nine out of 10 patients over their previous daily oral therapy in pivotal clinical trials. ViiV started shipping Cabenuva to U.S. wholesalers and specialty distributors in February.
In early May, ViiV Healthcare announced the initiation of a rolling submission of an NDA with the FDA for the long-acting injectable cabotegravir for the prevention of HIV, also known as pre-exposure prophylaxis (PrEP). ViiV was granted BTD for long-acting cabotegravir during November 2020 based on efficacy and safety results from the Phase IIb/III double blind study HPTN 083.
First soluble guanylate cyclase stimulator
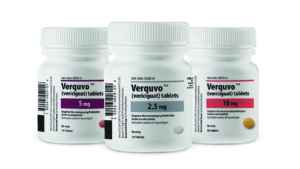
medicine white pill bottles isolated without shadow – photography; Shutterstock ID 1788779756; Purchase Order: –
The Jan. 19 marketing clearance of the potential blockbuster medicine Verquvo (vericiguat) marked the FDA’s first novel drug approval of 2021. As the first soluble guanylate cyclase (sGC) stimulator, Verquvo was approved to reduce the risk of cardiovascular death and heart failure hospitalization following a hospitalization for heart failure or need for outpatient intravenous (IV) diuretics in adults with symptomatic chronic heart failure and ejection fraction less than 45 percent.
The U.S. approval of Verquvo, which is the first treatment for chronic heart failure approved specifically for patients following a hospitalization for heart failure or need for outpatient IV diuretics, is based on the results of the pivotal Phase III VICTORIA study and follows a priority regulatory review. Verquvo (2.5 mg, 5 mg, and 10 mg tablets) is jointly developed by Merck & Co. and Bayer AG, which are sharing sales 50-50.
“Patients with symptomatic chronic heart failure and reduced ejection fraction have a high risk for hospitalization after experiencing symptoms of heart failure requiring outpatient IV diuretic treatment or hospitalization. By some estimates, more than half of these patients are rehospitalized within a month of discharge due to a worsening event and approximately one in five die within two years,” stated Dr. Paul W. Armstrong, cardiologist and Distinguished University Professor of Medicine at the Canadian VIGOUR Centre, University of Alberta, and study chair of the VICTORIA study.
The randomized, parallel-group, placebo-controlled, double-blind, event-driven, multi-center clinical trial VICTORIA (NCT02861534) compared Verquvo to placebo in 5,050 adult patients with symptomatic chronic heart failure (New York Heart Association [NYHA] class II-IV) and left ventricular ejection fraction (LVEF) less than 45 percent, following a worsening heart failure event. The study’s primary endpoint was a composite of time to first event of cardiovascular death or hospitalization for heart failure (HF). The primary endpoint’s median follow-up was 11 months. Verquvo was superior to placebo in reducing the risk of cardiovascular death or HF hospitalization based on a time-to-event analysis.
Bayer, which initially developed Verquvo, has previously touted peak sales of Verquvo at €1 billion. The drug’s market competition includes a pair of blockbuster SGLT2 inhibitors, Novartis’ Entresto and AstraZeneca’s Farxiga.
First anti-BCMA CAR T cell therapy for r/r MM
Among the FDA’s BLA approvals in 2021, Bristol Myers Squib and bluebird bio Inc. received U.S. approval on March 26 for Abecma (idecabtagene vicleucel; ide-cel) as the first B-cell maturation antigen (BCMA)-directed chimeric antigen receptor (CAR) T cell immunotherapy for the treatment of adult patients with relapsed or refractory (r/r) multiple myeloma (MM) after four or more prior lines of therapy, including an immunomodulatory agent, a proteasome inhibitor and an anti-CD38 monoclonal antibody. The personalized immune cell therapy is approved as a one-time infusion with a recommended dose range of 300 to 460 x 106 CAR-positive T cells. Abecma recognizes and binds to BCMA, a protein that is nearly universally expressed on cancer cells in MM, leading to the death of BCMA-expressing cells.
“CAR T cell therapies have shown transformational potential for the treatment of hematologic malignancies, and we, with our partners at bluebird bio, are proud to bring the first CAR T cell therapy to appropriate triple-class exposed patients with relapsed or refractory multiple myeloma, offering the chance for durable response,” stated Samit Hirawat, M.D., chief medical officer, Bristol Myers Squibb. “Bristol Myers Squibb is now the only company with two approved CAR T cell therapies with distinct targets of CD19 and BCMA. As our second FDA-approved CAR T cell therapy, Abecma underscores our commitment to deliver on the promise of cell therapies for patients who are battling aggressive and advanced blood cancers with limited effective treatment options.”
PDUFA REVIEWS ON THE HORIZON
The Prescription Drug User Fee Act (PDUFA) was created by Congress during 1992 and authorizes the FDA to collect fees from companies that produce certain human drug and biological products. Since the passage of PDUFA, user fees have played a significant role in expediting the drug approval process. Following are several PDUFA review dates scheduled during July-December 2021 for potential new medicines anticipated to shake up the U.S. marketplace.
Tenapanor
Ardelyx Inc.’s tenapanor is awaiting FDA approval for the control of serum phosphorus in adult patients with chronic kidney disease (CKD) on dialysis. Hyperphosphatemia represents a serious condition that is an independent predictor of morbidity and mortality in dialysis patients. Despite treatment with available medicines, 40 percent of patients continue to have phosphorous levels outside of target ranges in any given month.
With a unique mechanism of action, tenapanor acts locally in the gut to inhibit the sodium hydrogen exchanger 3 (NHE3). This results in a proposed conformational change of the epithelial cell tight junctions, thereby significantly reducing paracellular permeability to phosphate and decreasing phosphate absorption via this primary pathway.
The PDUFA for the tenapanor NDA was extended by three months to July 29, 2021. The NDA is supported by a comprehensive development program involving more than 1,000 patients, including three Phase III studies, each of which met their primary and key secondary endpoints. Ardelyx is conducting NORMALIZE, an extension study of the PHREEDOM Phase III monotherapy trial, which is designed to assess the ability of tenapanor (as monotherapy or in combination with sevelamer) to achieve serum phosphorus levels in the normal range in patients with CKD on dialysis.
Bimekizumab
Market expectations are high for UCB SA’s bimekizumab after the investigational humanized monoclonal IgG1 antibody outperformed the blockbuster medicines Stelara (J&J) and Cosentyx (Novartis) in clinical studies. Intended for the treatment of adults with moderate-to-severe plaque psoriasis, bimekizumab is under review by the U.S. FDA and the European Medicines Agency (EMA). The PDUFA date for UCB’s BLA for bimekizumab for treating adults with moderate-to-severe plaque psoriasis is set for Oct. 15, 2021. Regulatory reviews are additionally underway in Japan, Australia and Canada.
Bimekizumab selectively inhibits IL-17A and IL-17F, which are two key cytokines driving inflammatory processes. IL-17F has overlapping biology with IL-17A and drives inflammation independently to IL-17A, according to research. Selective inhibition of IL-17F in addition to IL-17A suppresses inflammation to a greater extent than IL-17A inhibition on its own. The safety and efficacy of bimekizumab are being assessed across multiple disease states as part of a robust clinical program. Bimekizumab is additionally being evaluated in Phase III clinical studies for potential indications in psoriatic arthritis, ankylosing spondylitis, non-radiographic axial spondyloarthritis and hidradenitis suppurativa.
Industry analysts have projected global 2026 sales of $1.63 billion for bimekizumab.
Efgartigimod
Argenx SE’s intravenous (IV) efgartigimod is on track to potentially become the first approved medicine within the FcRn antagonist drug class. The new drug candidate is intended for treating generalized myasthenia gravis (gMG).
Argenx announced on March 2, 2021, that the FDA accepted for review the BLA for efgartigimod. The U.S. regulatory agency set a standard 10-month review process with a PDUFA target action date of Dec. 17, 2021.
The BLA included results from the pivotal Phase III ADAPT study assessing the safety and efficacy of efgartigimod for treating gMG. ADAPT met the study’s primary endpoint defined as percentage of responders on the Myasthenia Gravis Activities of Daily Living (MG-ADL) score among acetylcholine receptor-antibody positive (AChR-Ab+) gMG patients. After completing ADAPT, 90 percent of participants entered ADAPT+, a three-year open-label extension study assessing the long-term safety and tolerability of efgartigimod.
Argenx on March 2 opened the pre-approval access (PAA) program in the United States, which enables eligible people living with gMG to receive treatment with efgartigimod. The purpose of the PAA is to open availability of an investigational treatment to individuals who have a high degree of unmet clinical need with gMG and are unable to participate in a clinical study.
The investigational antibody fragment efgartigimod is designed to reduce disease-causing immunoglobulin G (IgG) antibodies and block the IgG recycling process. Efgartigimod binds to the neonatal Fc receptor (FcRn), which is widely expressed throughout the body and plays a vital role in rescuing IgG antibodies from degradation. Blocking FcRn reduces IgG antibody levels representing a logical potential therapeutic approach for several autoimmune diseases known to be driven by disease-causing IgG antibodies, including myasthenia gravis, pemphigus vulgaris, immune thrombocytopenia (ITP) and chronic inflammatory demyelinating polyneuropathy (CIDP).
“Efgartigimod has the potential to help people living with gMG as well as several other severe autoimmune diseases mediated by IgG autoantibodies,” according to Tim Van Hauwermeiren, CEO of Netherlands-based biopharma company argenx. “Our team is advancing registrational trials across four indications with plans to start enrollment in two additional efgartigimod indications this year.”