U.S. plans for hundreds of millions of cheap, fast Covid-19 tests
U.S. plans for hundreds of millions of cheap, fast COVID-19 tests
(Reuters) – U.S. manufacturers are sharply increasing production of cheap, fast – but less accurate – COVID-19 tests, aiming for 100 million per month by year end that will enable schools and workplaces to significantly expand testing.
Manufacturing and government sources tell Reuters that more than half a dozen so-called antigen tests will likely be authorized by the end of October. U.S. regulators in recent months have authorized antigen tests from Abbott Laboratories ABT.N, Becton Dickinson & Co BDX.N, Quidel Corp QDEL.O and LumiraDX.
When planned production of the newly authorized tests are combined with previously approved diagnostics, overall monthly U.S. testing capacity will exceed 200 million per month by year end, these sources said.
Makers of the four recently-approved antigen tests have the capacity to make around 40 million per month, but expect to more than double that by year end, according to a Reuters analysis that includes proprietary figures shared by companies.
Unlike the $100 and up molecular diagnostics currently dominating U.S. testing that must be sent to a lab and often take several days for results, antigen tests can cost as little as $5. They can be performed anywhere and produce results in minutes.
That opens the possibility of regular screening at schools and businesses of even asymptomatic people, an important tool for containing future outbreaks, experts said.
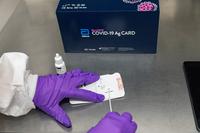
A healthcare professional adds the extraction reagent and a patient specimen to Abbott’s BinaxNOW COVID-19 Ag rapid test card in an undated photograph released by Abbott Labs in Abbott Park, Illinois, U.S. Abbott Labs/Handout via REUTERS
“If we could get testing to a scale where everyone you want to test can be tested quickly and cheaply with a quick turnaround time (for results), then you could screen people” before they spread the virus, said Dwayne Breining, director of labs at Northwell Health, New York state’s largest hospital system.
Lab-based molecular tests are too hard to make and deploy at that level, he said.
Antigen tests detect certain proteins that are part of the virus from samples taken via nasal or throat swabs, similar to rapid tests for strep throat in a doctor’s office.
RELIABILITY CONCERNS
A lack of testing capacity and little federal coordination early in the pandemic hampered efforts to control spread of the virus that has infected more than 6 million people in the United States.
Still, regulators and health experts are concerned about antigen test reliability. They typically detect the virus around 80% to 90% of the time, below the more than 95% rate of lab-based tests. False negative results raise the likelihood that sick people could unwittingly spread COVID-19.
There is also not enough data to be certain the new tests can detect the virus when infected people are in the early, pre-symptomatic stage, potentially limiting their usefulness.
The U.S. conducted around 25 million tests in August, including lab and antigen tests, according to data from the University of Oxford. Antigen test makers and their suppliers are gearing up for a huge boost.
Tony Lemmo, chief executive of BioDot Inc, which makes dispensers of chemicals used in the tests, says he has recently received orders that would translate into some 500 million tests in the coming months.
The United States could have capacity to conduct 3 million coronavirus tests per day this month, about half of them antigen tests. That could climb to as high as 135 million monthly tests in October, a top health official told a U.S. congressional panel on Wednesday.
European diagnostics companies Roche Holding AG ROG.S and Quiagen NV QIA.DE have said they will apply for U.S. authorization for their antigen tests.
The National Institutes of Health is working with companies on new tests that will likely add as many as another 30 million tests per month to overall capacity this year, a U.S. official told Reuters. The agency has also provided grants to help testmakers boost manufacturing capacity, including $71 million to Quidel in July.
The U.S. official, who was not authorized to speak publicly, told Reuters that getting to 100 million tests a month by year end could potentially slip by a couple of months because of production challenges.
To ramp up, companies need to hire enough skilled workers and source the paper used in the tests, called nitrocellulose, the official said.
“There’s just so much required to go from zero to millions of tests,” said Quidel CEO Douglas Bryant, whose company is working with large U.S. universities on daily testing of student athletes.
College football teams in the Big Ten conference will use antigen testing after announcing on Wednesday they would go ahead with games beginning next month.
Nursing homes are using Becton Dickinson’s antigen tests to screen residents and staff through a government program.
Even if testmakers succeed in scaling production, capacity will remain tight for some time, as schools, employers and others clamor for tests, executives and officials said.
Quidel has prioritized customer requests for its tests, Bryant said, with healthcare facilities and schools near the top, and industries like tourism further back in line.
Reporting by Carl O’Donnell; Editing by Caroline Humer and Bill Berkrot
Our Standards: The Thomson Reuters Trust Principles.
Reuters source:



