Monkeypox: experts urge caution, surveillance but stop short of declaring emergency
Monkeypox: experts urge caution, surveillance but stop short of declaring emergency
Published: Jul 21, 2022
By Gail Dutton
BioSpace
Will monkeypox be the next scourge on humanity or a blip on the radar screen of diseases? While the odds favor the latter – a serious but not pandemic-level health threat – scientists around the world are working to expand the knowledge base and the U.S. government is ramping up testing and vaccine availability.
What European Studies Show
A new study from the Barcelona Institute for Global Health at the University of Barcelona has found monkeypox in saliva, semen, urine, fecal matter and nasopharyngeal samples in about three-quarters of the dozen infected individuals who were tested. Each also had high levels of viral load in their monkeypox lesions. This study, published in Eurosurveillance, showed that “DNA is frequently present in various biological fluids, particularly saliva, during the acute phase of the disease, and up to 16 days after the onset of symptoms in one patient,” first author Aida Peiró-Mestres said in a statement. A high viral load suggests infectious potential. The next step is to isolate infectious virus from the samples.
Of the 12 patients Peiró-Mestres and colleagues examined, six were in their 30s, five in their 40s and one was in his 50s. Only four of the patients had previously been vaccinated for smallpox. Two had syphilis, four had HIV and eight had between five and ten sexual partners in the previous month. The remainder reported having fewer than five partners the prior month. All patients were men who have sex with men.
Another article in the same journal analyzed 508 cases of transmission in Madrid and 521 cases in Berlin. In Madrid, most of those reported cases involved men who had sex with other men. Many of them frequented the same sauna in central Madrid. In Berlin, at the beginning of the outbreak, the infections were acquired while traveling abroad but from late May onward, locally-acquired infections became the most frequent. In both Madrid and Berlin, patients who acquired monkeypox during travels most often mentioned the Maspalomas Gay Pride festival on Gran Canarie.
The virus appears not to be transmitted sexually. Instead, as Johns Hopkins School of Medicine notes on its advisory page, “Monkeypox is spread by close contact and exposure to an infected person’s respiratory droplets, skin lesions or other bodily fluids…It is more likely to affect people who have never been vaccinated against smallpox.” However, since routine vaccination against smallpox ended in 1972 in the U.S., there’s no definitive word on how effective those older vaccinations may be against monkeypox. The Centers for Disease Control and Prevention (CDC) recommends booster shots every three years for medical personnel and lab workers who still receive smallpox vaccinations.
Rate of Monkeypox Spread Concerning
Monkeypox is not likely to become a major public health threat, despite the growing numbers of infections outside its endemic regions. “Monkeypox is very different than COVID,” White House Coronavirus Coordinator Ashish Jha said on PBS.
While “Monkeypox is not the most concerning epidemic, it does need to be considered seriously as it could pose problems to many,” Erica Susky, an infection control practitioner in hospital epidemiology in Toronto, and an instructor in microbiology and infectious disease for Infection Prevention and Control (IPAC) Canada’s “Essentials of IPAC” course told BioSpace.
As of Wednesday, there were 2,108 confirmed cases of monkeypox in the U.S. and 14,000 throughout the world, according to the World Health Organization. Five deaths have occurred so far, all in Africa. Monkeypox cases are increasing in number, but mass vaccination isn’t required, according to the latest guidance from the WHO.
“The number of cases may not seem troubling now, but the increasing rate of its spread is cause for serious concern. It may indicate that the current strain of monkeypox is more contagious than previously thought,” David Culpepper, M.D., clinical director of LifeMD, a direct-to-patient telehealth company, told BioSpace.
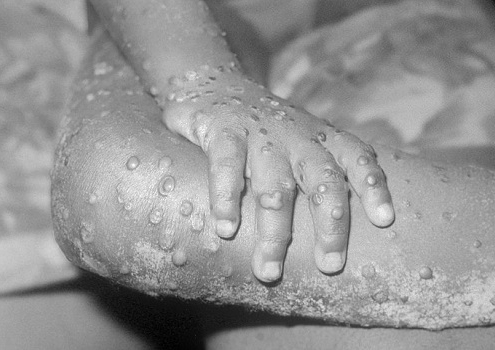
Because monkeypox is still relatively rare, it may at first be diagnosed as chickenpox, measles or syphilis. It starts with a general blasé feeling before proceeding to fever and muscle aches – like the flu – followed by swollen lymph nodes and, a few days later, a blister-like rash that spreads and persists for one or two weeks. “Though monkeypox does not spread as readily as COVID-19, the period during which the virus can spread to another is much longer, starting at the initial stage of illness and continuing until all of the lesions or scabs have all fallen off, which can be as long as 28 days,” Susky said.
Is the United States Adequately Prepared?
There are two strains of monkeypox – the West African strain (which is fueling this outbreak) and the Congo basin strain. “The West African clade is the less fatal of the two clades with a fatality of 1%, but it could still pose more serious symptoms and complications in at-risk groups,” Susky explained. “Those at a higher risk of a serious monkeypox infection include immune-compromised individuals, children under four years of age and the elderly. Serious complications include encephalitis, secondary bacterial infections and sepsis and corneal infections causing blindness.”
In the U.S., only one vaccine is approved for monkeypox (and smallpox) – Jynneos, by Bavarian Nordic. The U.S. Department of Health and Human Services just ordered 2.5 million doses of the Jynneos vaccine, with arrival set for 2023. By the end of July, however, 780,000 doses of Jynneos are expected to arrive on U.S. soil from Denmark, where they are being stored by the supplier.
Another vaccine, ACAM2000 was approved as a smallpox vaccine and, therefore, should be effective against monkeypox. It should not be used in people with weakened immune systems or eczema.
“The vaccine is an important tool to prevent the spread and severity in at-risk groups and those that have been exposed to the virus,” Susky said. “Predicting (the spread of the virus) will be key in determining how much vaccine should be ready and at what time. Watching the numbers of people newly acquiring monkeypox, their population or risk groups, and the ensuing number of people exposed will guide decisions on how much vaccine to produce in the coming months.”
The CDC can now test up to 70,000 clinical samples per week.
“Monitoring the effectiveness of the vaccine in preventing severe cases and spread, and the virulence of the current outbreak, also will assist in determining the overall benefit of creating the needed supply of vaccine,” Susky noted.
To that end, the WHO is hosting a webinar July 27th to discuss the spread of monkeypox and what is known to date.
Source: BioSpace

 BioSpace
BioSpace






 Reuters
Reuters